Edema Fluid Drainage and Swelling in Legs – Reduce Swelling
Edema Fluid Drainage and Swelling in Legs (🔥INSTANT COMFORT!) Reduces Swelling, Eases Stiffness, Relaxes Muscles, and Supports Long Sitting Felief.
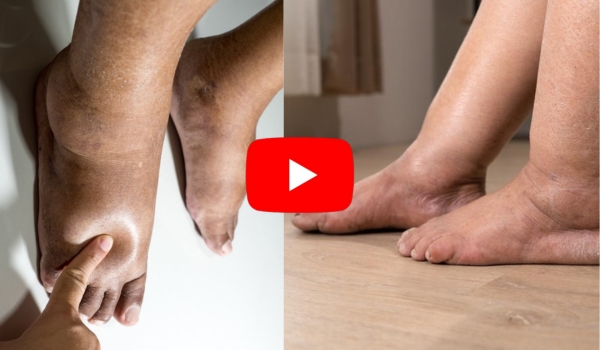

Swelling in the legs, medically known as edema, is a common health concern that affects millions of people worldwide.
Edema occurs when excess fluid accumulates in the tissues, particularly in the lower extremities, leading to discomfort, stiffness, and limited mobility.
This condition can result from a variety of factors, including prolonged sitting, underlying medical conditions, poor circulation, or even dietary habits.
In this comprehensive guide, we will explore what edema is, how it works, the scientific explanation behind it, methods to manage it, and tips to ensure healthier legs.
What Is Edema and Swelling in Legs?
Edema refers to the abnormal accumulation of fluid in the tissues, which leads to swelling.
While edema can occur anywhere in the body, it is most commonly noticed in the legs, ankles, and feet because gravity causes fluid to settle in the lower extremities.
Swelling may be mild, causing temporary discomfort, or severe enough to impact mobility and quality of life.
Leg edema may present with the following symptoms:
-
Puffiness in the legs or ankles
-
Tightness of shoes or socks due to swelling
-
Stiffness or heaviness in the legs
-
Shiny or stretched skin over the swollen area
-
Reduced flexibility or mobility
The condition is not just cosmetic. If left unmanaged, persistent edema can lead to pain, skin changes, and even complications such as infections or ulcers. Understanding edema is the first step toward effective management.
How Edema and Fluid Accumulation Work?
Edema occurs when excess fluid builds up in the tissues, most commonly in the legs, ankles, and feet.
Under normal conditions, the body maintains a delicate balance between fluid entering the tissues from blood vessels and fluid returning to circulation or being drained by the lymphatic system.
Disruption of this balance leads to fluid accumulation, causing swelling, heaviness, and stiffness.
Capillary Filtration
- Blood flows through tiny vessels called capillaries, which allow water, salts, and nutrients to pass into surrounding tissues.
- When fluid leaves the capillaries faster than it can return to circulation, it accumulates in the tissues, causing visible swelling.
Lymphatic Drainage
- The lymphatic system acts as a secondary drainage network, collecting excess tissue fluid and returning it to the bloodstream.
- If lymphatic vessels are blocked or inefficient, fluid pools in the tissues, worsening edema.
Venous Return
- Veins in the legs carry blood back to the heart. Weak veins, damaged valves, or prolonged inactivity can reduce blood flow, allowing fluid to settle in the lower extremities.
- This is why leg edema is common in sedentary individuals or those standing for long periods.
Gravity Effect
- Gravity naturally pulls fluid downward. When standing or sitting for long periods, fluid tends to accumulate in the lower limbs, increasing swelling and discomfort.
Protein Imbalance
- Proteins in the blood, like albumin, maintain osmotic pressure, keeping fluid inside the blood vessels. Low protein levels reduce this ability, causing fluid to leak into tissues and creating edema.
Inflammation and Injury
- Inflammatory responses from injury, infection, or chronic conditions like heart, kidney, or liver disease increase capillary permeability.
- This allows proteins and water to escape into surrounding tissues, leading to localized swelling.
The Science Behind Edema Fluid Drainage and Swelling in Legs
Scientific research shows that edema is influenced by multiple factors, including vascular permeability, inflammation, and fluid imbalance.
Vascular Permeability
- Edema occurs when capillary walls become overly permeable, often due to inflammation. Proteins and water leak into surrounding tissues, causing swelling.
- Conditions like venous insufficiency worsen this, highlighting the importance of healthy blood vessels in fluid balance.
Inflammatory Response
- Injuries, infections, or chronic conditions like heart or kidney disease trigger inflammation, increasing fluid leakage into tissues.
- This results in localized swelling, stiffness, and discomfort, making edema both a functional and visible problem.
Gravity Effect
- Legs are prone to swelling because gravity causes fluid to pool in the lower extremities. Sedentary lifestyles or prolonged standing reduce muscle pumping, worsening fluid accumulation.
- Elevation and movement help counteract this effect and improve circulation.
Protein Imbalance
- Low plasma protein levels, especially albumin, reduce the blood’s ability to retain fluid. This causes water to seep into surrounding tissues, leading to edema.
- Malnutrition, liver, or kidney issues often contribute to this protein imbalance.
Lymphatic Drainage
- The lymphatic system collects excess tissue fluid and returns it to the bloodstream. When blocked or weakened, fluid builds up, especially in the legs.
- Therapies like manual lymphatic drainage and compression can enhance lymph flow and reduce chronic swelling.
Scientific Evidence
- Studies show that combining movement, leg elevation, and targeted therapies improves circulation and reduces fluid buildup.
- Walking, calf exercises, compression, and massage effectively manage edema, addressing both causes and symptoms.
How to Use Edema Fluid Drainage to Reduce Leg Swelling?
Managing edema and leg swelling effectively involves combining lifestyle habits, exercises, and supportive therapies. Here’s how to use these strategies for the best results:
Leg Elevation
-
Lie down and raise your legs above heart level using pillows or a wedge.
-
Keep legs elevated for 15–20 minutes, 2–3 times daily.
-
This helps fluid flow back toward the heart, reducing swelling and stiffness.
Compression Therapy
-
Wear compression stockings or sleeves that fit snugly but comfortably.
-
Use daily as directed, especially during prolonged standing or sitting.
-
Compression improves venous return, preventing fluid pooling in the legs.
Movement and Exercise
-
Perform ankle pumps, calf raises, or short walks throughout the day.
-
Even simple leg stretches every hour stimulate circulation and lymph drainage.
-
Regular activity strengthens the calf muscles, acting as a natural pump to reduce fluid buildup.
Manual Lymphatic Drainage (MLD)
-
Gentle massage techniques can help move excess fluid from the legs back into circulation.
-
Can be done professionally or with guidance for home use.
-
Focus on upward strokes toward the groin to follow natural lymph pathways.
Hydration and Diet
-
Drink plenty of water to maintain fluid balance.
-
Reduce high-sodium foods that encourage water retention.
-
Eat foods rich in potassium and protein to support vascular health and prevent fluid accumulation.
Cold Therapy
-
Apply a cool compress to swollen areas for 10–15 minutes.
-
This reduces inflammation, eases discomfort, and relieves stiffness.
Lifestyle Adjustments
-
Avoid prolonged sitting or standing. Take short walking breaks every hour.
-
Wear comfortable shoes that do not restrict circulation.
-
Maintain a healthy weight to lower pressure on leg veins.
Regular Monitoring
-
Check for persistent or worsening swelling.
-
If swelling does not improve or is accompanied by pain, redness, or heat, consult a doctor to rule out heart, kidney, or vascular issues.
Why Edema Fluid Drainage Works?
Fluid drainage methods work because they target the root causes of swelling.
- Better Venous Circulation: Elevation and compression support healthy blood flow, helping prevent fluid from collecting in the legs.
- Improved Lymphatic Drainage: Massage techniques and light exercises encourage lymph movement, minimizing fluid buildup.
- Balanced Fluid Levels: Proper hydration and a nutrient-rich diet help regulate electrolytes and water balance, limiting fluid retention.
- Natural Muscle Pump Action: Consistent movement activates calf muscles, which help push excess fluid back toward the heart.
- Reduced Inflammation: Soothing massage, cooling methods, and anti-inflammatory approaches ease swelling and improve tissue flexibility.
Scientific studies confirm that combining multiple techniques, such as compression, exercise, and elevation, offers the most effective results in reducing leg edema.
Benefits of Edema Fluid Drainage
Proper management of edema not only alleviates swelling but also enhances overall leg health. Key benefits include:
- Reduced Swelling and Discomfort: Effective edema management quickly eases leg heaviness, puffiness, and discomfort, providing relief and restoring comfort for daily activities and prolonged standing or sitting.
- Improved Mobility: By decreasing stiffness and fluid buildup, edema management enhances leg flexibility, making walking, climbing stairs, and daily movement easier and less tiring.
- Prevention of Complications: Proper fluid drainage lowers the risk of infections, ulcers, and venous insufficiency, protecting skin and veins while preventing serious long-term leg health issues.
- Enhanced Circulation: Managing edema supports blood flow and lymph drainage, promoting healthy circulation, reducing pooling of fluid, and supporting cardiovascular and vascular function.
- Better Sleep and Comfort: Reducing leg swelling and discomfort improves overall relaxation, allowing restful sleep and preventing nighttime cramps, heaviness, or pain in the lower extremities.
- Long-Term Vascular Health: Consistent edema care maintains vein and artery health, improves circulation long-term, and reduces the risk of chronic swelling, varicose veins, and vascular complications.
Additional Tips for Managing Leg Swelling
For long-term edema management, consider incorporating these additional strategies:
Avoid Prolonged Sitting or Standing
- Take regular breaks every hour to walk, stretch, or move your legs. This prevents fluid pooling, reduces swelling, and improves circulation.
Elevate Legs During Sleep
- Use pillows to slightly raise your legs while sleeping. Elevation aids fluid drainage, reduces nighttime swelling, and promotes leg comfort.
Wear Proper Footwear
- Choose shoes that fit comfortably and don’t restrict blood flow. Proper footwear supports circulation and helps prevent leg swelling and discomfort.
Maintain a Healthy Weight
- Keeping a healthy weight reduces pressure on leg veins, prevents fluid buildup, and lowers the risk of chronic swelling and vascular issues.
Regular Check-Ups
- Persistent leg swelling may signal heart, kidney, or vascular problems. Regular check-ups help detect issues early and prevent complications.
Cold Therapy
- Applying a cool compress to swollen legs reduces inflammation, soothes discomfort, and provides fast relief from stiffness and heaviness.
Herbal Support
- Natural remedies like ginger, turmeric, and green tea may boost circulation, reduce mild inflammation, and support overall leg health.
- Combining these habits with structured edema management techniques ensures faster relief and long-term leg health.
Final Thoughts
Edema and swelling in the legs are more than just a minor inconvenience; they are signs that the body is struggling with fluid balance.
Understanding the science behind edema, implementing fluid drainage methods, and adopting healthy lifestyle habits are key to managing this condition effectively.
For persistent or severe edema, medical evaluation is essential to rule out underlying conditions.
Consistent care not only alleviates immediate symptoms but also supports long-term vascular health, mobility, and comfort.
By prioritizing leg health and using scientifically backed techniques, edema can be effectively managed, allowing individuals to regain freedom of movement, comfort, and confidence in their daily lives.
Edema fluid drainage is not just about reducing swelling; it’s about restoring balance, function, and well-being. With the right knowledge, methods, and habits, healthy, comfortable legs are achievable for everyone.

.
.
.